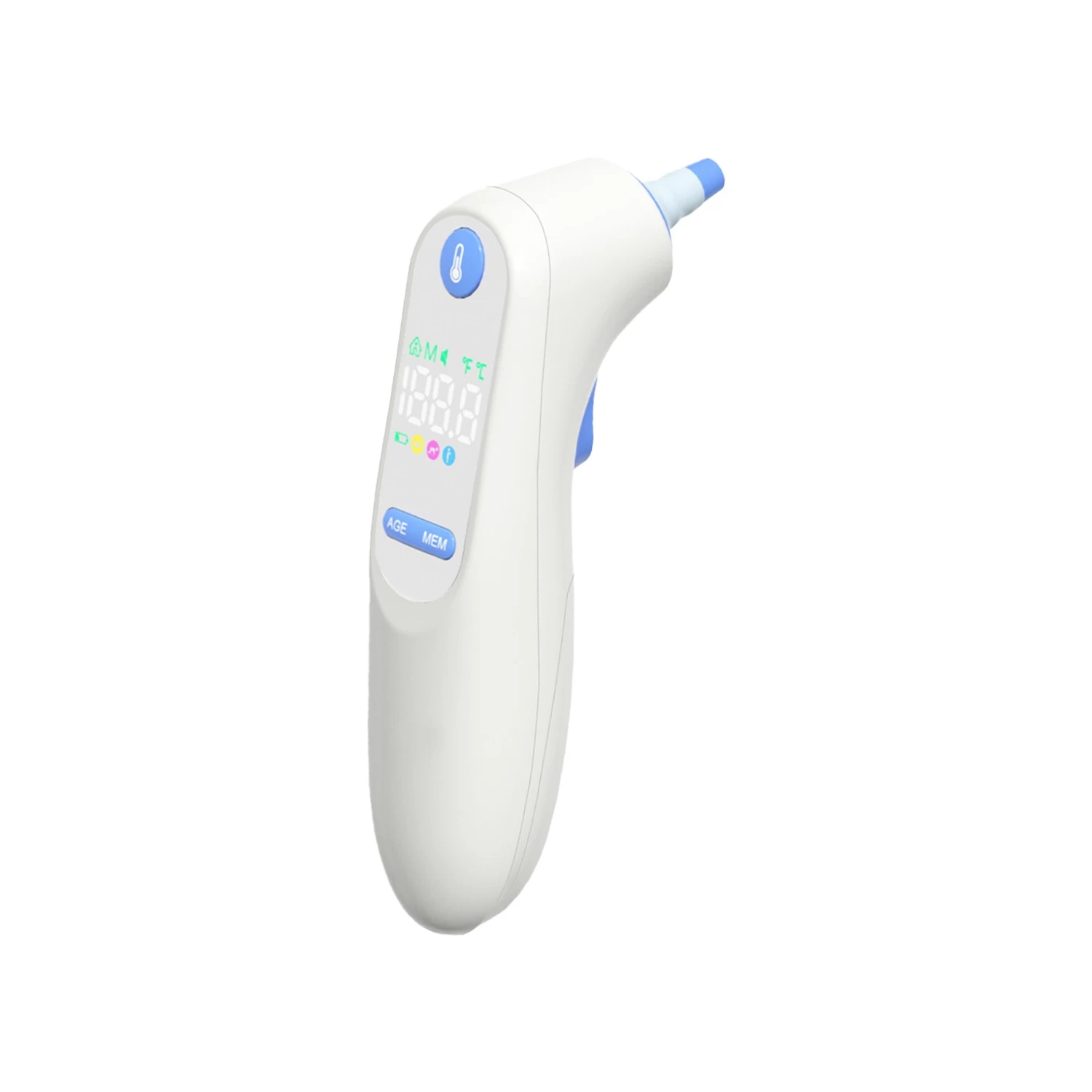
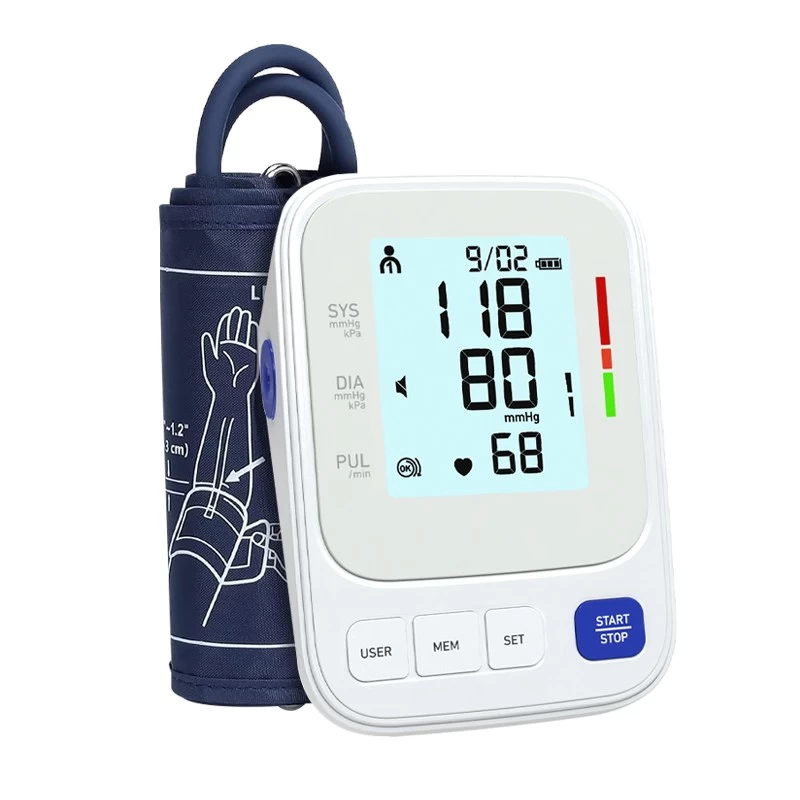
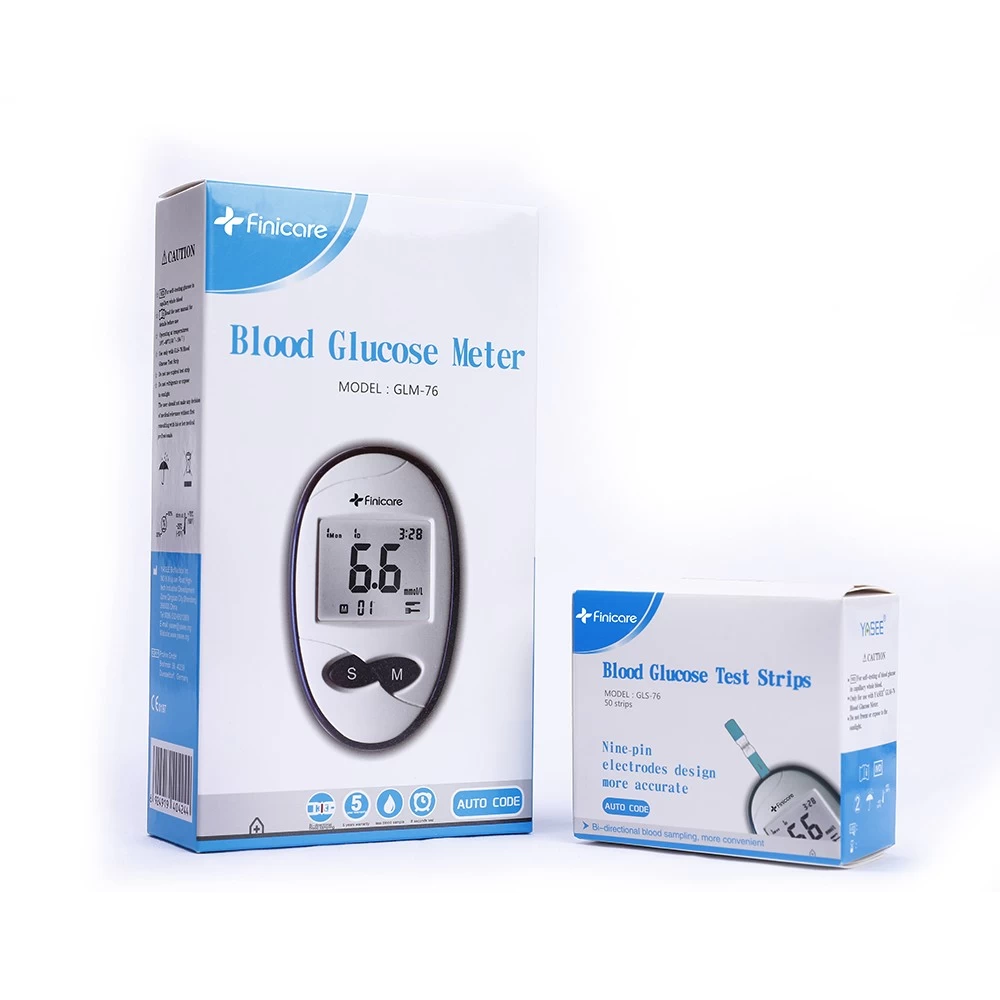
How Cellular IoT Is Solving the Oldest Problem in Household Medical Devices
Data That Never Arrives Is Data That Never Existed
The promise of household medical devices rests on one deceptively simple requirement: the data they capture must actually reach a clinician's screen. The sensors work. The algorithms work. But somewhere between the bedside and the cloud, readings vanish—silently, repeatedly, and without anyone noticing until it's too late. This isn't a hardware problem. It's a connectivity problem. And it has persisted for over a decade because the industry kept grafting consumer wireless standards onto a use case they were never built for.

The Bluetooth Detour
Consider the path a single blood pressure reading must travel in a typical Bluetooth-based system. The cuff captures the measurement. It searches for a paired smartphone. The smartphone must be nearby, powered on, running the correct app, with Bluetooth enabled and permissions intact. The app must successfully receive the data, then relay it over the phone's internet connection to a remote server.
That is five dependencies for one reading.
Any engineer will tell you that a chain with five links breaks more often than a chain with one. And in practice, it breaks constantly. Phones get left in another room. Apps get killed by aggressive battery optimization. Bluetooth pairings corrupt after software updates. The user—often elderly, often alone—has no way of knowing the transmission failed. The device screen says "complete." The cloud says nothing arrived. For household medical devices that are supposed to provide continuous care, this architecture is fundamentally flawed.
Wi-Fi: Better, but Still Fragile
Wi-Fi eliminates the smartphone middleman but introduces its own fragility. It demands a functioning home network—a router that stays online, a password the user can enter (often on a device with no keyboard), and signal coverage that reaches wherever the device is used. For a patient monitoring vitals from bed, a router two rooms away may as well be two miles away.
In rural and low-income settings, the situation is starker. Roughly 24 million Americans still lack reliable broadband access. For these populations, Wi-Fi-dependent household medical devices are not monitoring tools—they are paperweights.
LTE-M: One Link, No Breaks
4G LTE-M was purpose-built for exactly this scenario. It is a cellular protocol optimized not for streaming video or browsing the web, but for transmitting small, critical packets of data from low-power devices over long distances and through dense building materials.
An LTE-M-enabled device ships with a SIM embedded in the hardware. The user turns it on. It connects. There is no network to join, no password to enter, no phone to pair, no app to install. The reading travels from sensor to cell tower to cloud in a single, unbroken line. For the next generation of household medical devices, this represents the architectural reduction of a five-link chain to one.
Designing for the Person Who Won't Read the Manual
Every consumer product has a user who will never read the manual. In home health, that user is the majority. They are 78 years old. They have three medications and a cardiologist who wants daily blood pressure readings. They do not know what Bluetooth is. They should not have to.
The design philosophy behind cellular-connected household medical devices starts from this reality. The goal is not to make setup "easier"—it is to make setup nonexistent. When a device requires zero configuration, the gap between "unboxed" and "operational" collapses to nothing. Adoption rates rise not because the marketing improved, but because the friction disappeared.
This matters disproportionately for the populations that need monitoring most: the elderly, the chronically ill, those living alone, and those in medically underserved regions. Cellular connectivity doesn't just improve the user experience for these groups—it makes the user experience possible in the first place.
Continuity as a Clinical Asset
Intermittent data is not merely incomplete data. It is potentially deceptive data. A blood pressure log with unexplained gaps can mask dangerous trends. A heart rhythm record with missing hours might omit the exact window in which Atrial Fibrillation occurred. Clinicians trained to interpret continuous datasets are forced instead to extrapolate from fragments—a practice that introduces uncertainty precisely where precision matters most.
Cellular-enabled household medical devices eliminate the most common causes of data gaps. Because each reading is sent the instant it is captured, there is no local buffer that overflows, no sync process that the user must trigger, and no dependency on a third-party device being available at the right moment. The result is a longitudinal health record that closely approximates what would be captured in a clinical setting—without requiring the patient to be in one.
The Shift Underway
The movement from Bluetooth and Wi-Fi to cellular connectivity is not a technology trend. It is a correction. For years, the industry tolerated a connectivity model that worked well enough in demos and marketing materials but failed quietly in the homes of the people who needed it most.
LTE-M does not add a feature to household medical devices. It removes a flaw—the fundamental assumption that the patient's home network and personal devices are reliable components of a medical data pipeline. They never were. Now they don't have to be.